In my years of practice, I have heard the same question from adult patients many times. They ask me, isn’t this just for kids? It is a fair question. Sealants have been marketed as a children’s treatment for years.
But after seeing thousands of mouths, I can tell you adults benefit from sealants more often than people realize. The answer of whether they are worth it depends on your mouth, your habits, and your cavity history.
What Are Dental Sealants?
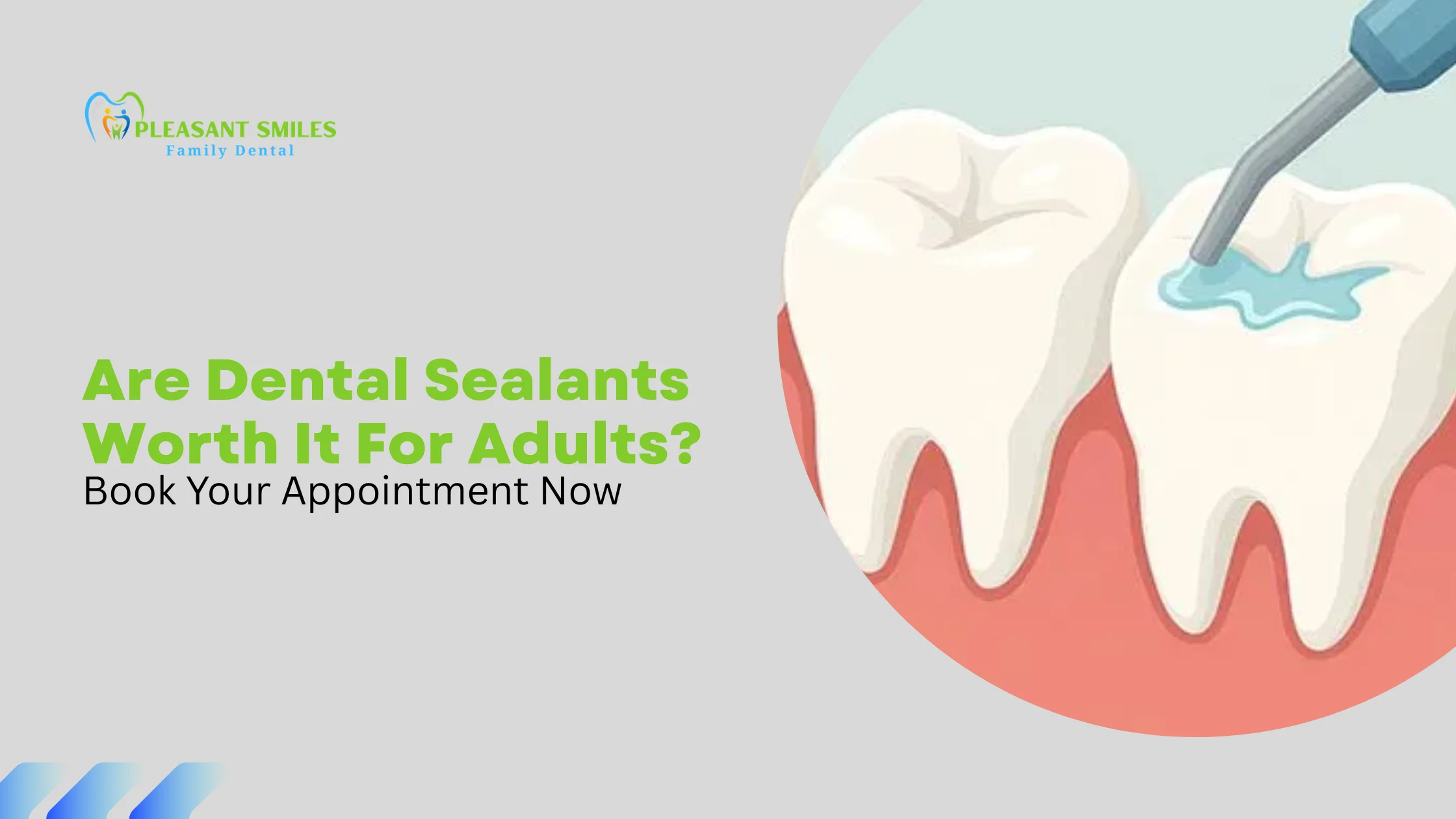
A dental sealant is a thin coating placed on the chewing surface of your back teeth. It fills the deep grooves where food and bacteria like to settle. Once it is in place, the tooth becomes easier to clean.
The material is a tooth colored resin, so nobody will see it when you talk or smile. Most patients tell me they forget it is even there after the first day.
A sealant is not a replacement for brushing or flossing. It is a backup for the spots that careful brushing has trouble reaching.
Dental Sealants: How Do They Work?
Placing a sealant is one of the easiest things we do in the office. The whole appointment takes about ten to fifteen minutes per tooth. There is no drilling, no shots, and no soreness afterward.
First I clean the tooth so nothing gets trapped under the coating. Then I apply a mild gel that roughens the surface so the sealant can grip. After a quick rinse, I paint the sealant on and harden it with a small curing light.
Once it cures, the sealant forms a smooth barrier over the chewing surface. Bacteria and food slide off instead of sinking into the cracks. The CDC and ADA both recognize sealants as an effective way to reduce decay on molars.
What’s the Difference Between Getting a Sealant as an Adult Compared to a Child?
The sealant material is the same for both. What changes is the reason for placing one.
With kids, the goal is simple. Their permanent molars come in around ages six and twelve, and most children are still learning how to brush well. We seal early to lock in protection before any damage starts.
With adults, I take a different approach. Some teeth may already have fillings or crowns, which means a sealant has nothing natural to bond to. Other teeth might still be in great shape but have grooves that trap food every day.
Instead of asking how old you are, I look at your cavity risk. That tells me far more than your age does. There is also a practical difference. Most insurance covers sealants for kids only, so adults usually pay out of pocket.
What Are the Pros of Dental Sealants For Adults?
Here are the main benefits I see in my adult patients:
- Cavity protection in spots that are hard to clean, even with careful brushing.
- Quick and painless procedure with no numbing, no drilling, and no recovery time.
- Far less expensive than a filling, and much cheaper than a crown or root canal down the line.
- Helps reduce repeat cavities in teeth that have been trouble spots before.
- Can ease mild sensitivity to cold or heat by covering the chewing surface.
- A gentle option for patients who feel anxious about other dental work.
What Are the Cons of Dental Sealants For Adults?
I always give my patients the full picture. Here are the honest downsides:
- Sealants do not last forever. They wear down over time, especially with grinding.
- Most insurance plans cover sealants for children only. Adults usually pay out of pocket.
- If a tooth has hidden decay, sealing over it traps the bacteria. A careful exam first prevents this.
- Some patients feel a slight bite difference for a day or two. It usually settles in on its own.
- Sealants only work on natural tooth surfaces. Teeth that already have fillings or crowns are not candidates.
Are Dental Sealants Worth It For Adults?
Here is the honest answer I give in my chair. Sealants are absolutely worth it for some adults and not really needed for others. Your personal cavity risk is what tips the scale.
You are a strong candidate if a few of these apply to you:
- You have had cavities show up in your back teeth more than once.
- Your molars have deep grooves you can feel with your tongue.
- You take medication that causes dry mouth.
- You drink coffee, soda, or sports drinks regularly.
- You wore braces or other orthodontic work that makes some teeth harder to clean.
- You deal with acid reflux or GERD, which can wear down enamel.
If three or more of these sound like you, sealants are usually a smart investment. If none of them apply and your adult cavity history is clean, you may not need them at all.
Are Dental Sealants Worth It For Kids?
Parents ask me this almost as often as adults do. My answer is usually a simple yes, but with a little context. Sealants for kids are one of the most cost effective preventive treatments in dentistry.
The best window to seal a child’s tooth is right after a permanent molar comes in. The first set shows up around age six, and the second set comes in around age twelve. Sealing soon after eruption keeps food and bacteria from settling into those deep grooves.
Children also benefit because their daily diets often include sticky and sugary foods. Crackers, juice, and fruit snacks cling to back teeth longer than parents would guess. A sealed molar gives those foods nowhere to hide.
Insurance is another reason I recommend sealants for kids. Most plans cover them for children up to a set age, often with little or no out of pocket cost. So you get strong protection at the most affordable price.
There are still cases where I do not seal a child’s tooth. If a tooth already has decay or a filling, a sealant is not the right call for that one. We treat the problem first, then seal the healthy molars around it.
When Sealants Are NOT Worth It for Adults
This is where most articles online get vague, and I think that does patients a disservice. Let me be specific about when I tell adult patients to skip sealants.
If your back teeth already have fillings or crowns, sealants are not the right tool. They only bond to the natural tooth surface, so there is nothing for them to grip on a restored tooth.
If there is any sign of active decay, we handle that first. Sealing over a cavity makes the problem worse, not better. And if your hygiene is solid and your cavity history is clean, the money may be better spent on other care.
Honest dentistry means saying no when no is the right answer. If sealants do not fit your situation, I will tell you so.
How Long Sealants Last and Signs Yours Are Failing
Sealants are designed to last for years, but no dental material lasts forever. How long yours holds up depends on your bite, whether you grind at night, your diet, and your checkup routine.
Between visits, watch for these signs that a sealant is starting to give out:
- Food starts getting stuck in a tooth that used to feel smooth.
- The chewing surface feels rough or sharp on your tongue.
- A tooth that had been comfortable feels sensitive again.
- You can see a chip, a gap, or a darker edge in the mirror.
If a sealant has worn down, there is no need to worry. Reapplying one is just as fast and painless as the first time. Routine cleanings every six months are the easiest way to keep tabs on your sealants.
Schedule an Appointment For Dental Sealants For Adults
Sealants are one of the simpler ways to protect your back teeth, but they are not right for everyone. The best place to start is a quick exam where we can look at your molars and talk through your cavity history.
At Pleasant Smiles Family Dental in Cheshire CT, I take time with every patient to explain what is needed and what is not. No upselling. No scare tactics. Just a clear plan based on your mouth.
Call our office at 860 426 0997 or visit by 1090 Meriden Waterbury Turnpike, Suite 2, Cheshire, CT 06410. New patients are always welcome, and we will find a time that fits your schedule.
Frequently Asked Questions
What are dental sealants?
A dental sealant is a thin, tooth-colored resin coating placed on the chewing surface of back teeth. It fills the deep grooves where food and bacteria settle, making the tooth easier to clean. Sealants are not a replacement for brushing or flossing — they act as a backup for spots that careful brushing has trouble reaching.
How do dental sealants work?
Placing a sealant takes about 10 to 15 minutes per tooth with no drilling, no shots, and no soreness. The dentist cleans the tooth, applies a mild gel to roughen the surface, rinses it, paints on the sealant, and hardens it with a curing light. Once cured, it forms a smooth barrier so bacteria and food slide off instead of sinking into the cracks.
What is the difference between getting a sealant as an adult versus a child?
The material is the same. With kids, sealants are placed on newly erupted permanent molars (around ages 6 and 12) before any decay starts. With adults, the focus shifts to cavity risk rather than age. Some adult teeth already have fillings or crowns and can’t be sealed, while others are healthy but have deep grooves that trap food. Most insurance covers sealants only for children, so adults typically pay out of pocket.
What are the pros of dental sealants for adults?
Sealants protect cavity-prone areas that are hard to clean, the procedure is quick and painless with no numbing or recovery time, they cost far less than a filling or crown, they help reduce repeat cavities in trouble teeth, they can ease mild sensitivity to hot or cold, and they’re a gentle option for patients who feel anxious about dental work.
What are the cons of dental sealants for adults?
Sealants do not last forever and wear down over time, especially with grinding. Most insurance plans cover them only for children, so adults usually pay out of pocket. If a tooth has hidden decay, sealing over it traps the bacteria — a careful exam first prevents this. Some patients feel a slight bite difference for a day or two. Sealants also only work on natural tooth surfaces, so teeth with fillings or crowns are not candidates.
Are dental sealants worth it for kids?
Yes, Sealants are one of the most cost-effective preventive treatments in dentistry for children. The best window is right after a permanent molar erupts, around ages 6 and 12. Most insurance plans cover sealants for children with little or no out-of-pocket cost. The exception is a tooth that already has decay or a filling, which is treated first before sealing the healthy molars.
How long do dental sealants last and how do I know if mine are failing?
Sealants are designed to last for years, but longevity depends on your bite, grinding habits, diet, and checkup routine. Signs a sealant is wearing out include food getting stuck in a tooth that used to feel smooth, a rough or sharp surface on the tongue, returning sensitivity, or a visible chip or darker edge. Reapplying a sealant is just as quick and painless as the first time.